While in my essay on obesity I argued that the obese suffer from defective glucose metabolism in the muscles, it appears that children with ADHD suffer from the exact opposite problem: very efficient glucose metabolism. Insulin is critical for the metabolism of glucose. When insulin levels are high, body fat cells are unable to release their fat stores, as shown in the figure at the right [lipolysis = breakdown of fat tissue]. I have proposed that obesity is protective
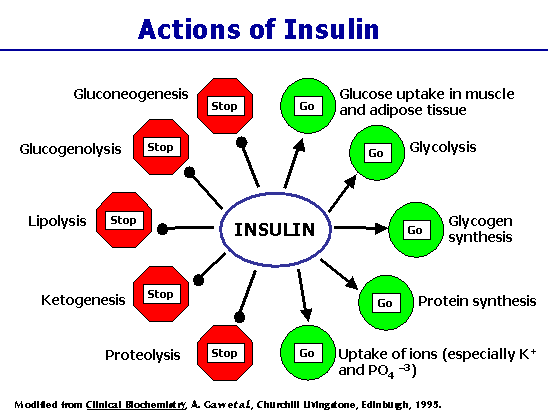 against ADHD because the abundant fat cells can release plenty of triglycerides into the blood early in the morning, before the first meal. This fat supply can tide the person over through the long fatty-acid drought that occurs during the day, while an abundance of high-glycemic index low-fat foods are consumed. A further advantage is that obese people typically have reduced insulin production (due to insufficient calcium, which I explain later), so the levels of insulin in the blood are never excessively high. Their muscle cells have been programmed to prefer fat metabolism, but there is also plenty of fat available from the triglycerides (released before the meal began) to supply the brain's raw materials to enhance communication through neural pathways. Furthermore, the glucose that is not consumed by the muscles is readily available
against ADHD because the abundant fat cells can release plenty of triglycerides into the blood early in the morning, before the first meal. This fat supply can tide the person over through the long fatty-acid drought that occurs during the day, while an abundance of high-glycemic index low-fat foods are consumed. A further advantage is that obese people typically have reduced insulin production (due to insufficient calcium, which I explain later), so the levels of insulin in the blood are never excessively high. Their muscle cells have been programmed to prefer fat metabolism, but there is also plenty of fat available from the triglycerides (released before the meal began) to supply the brain's raw materials to enhance communication through neural pathways. Furthermore, the glucose that is not consumed by the muscles is readily availableIt seems that ADHD children have adopted an entirely different strategy for coping with insufficient fats in the food sources. Research has shown that many of them suffer from hypoglycemia (low blood sugar), because their insulin is extremely efficient -- the opposite of diabetes [19]. In direct contrast with obese people, the fat cells of ADHD children program the muscles to prefer glucose over fat as a fuel source. This reduces the burden placed on the fat cells to convert glucose to fat, which is a very inefficient process. Furthermore, unlike the obese, ADHD children typically have no shortage of insulin, produced by the pancreas in response to glucose. Insulin enables the muscles to readily consume the glucose, but also unfortunately supresses the ability of the fat cells and the liver to release stored fats. If there is plenty of glucose in the consumed foods, and very little fat, then the muscles and brain consume the glucose, but the brain is deprived of sufficient fats to construct high quality long-distance neural connections. ADHD children have been found to have shrunken white matter in parts of the brain that are involved with focus of attention and learning new knowledge. I believe this is a direct consequence of a lack of a supply of fats, critically, when the neural pathways that make up the white matter are actively being formed.
The body with inadequate fat supply in the food sources is essentially like a car engine running on only two cylinders. While it has been argued that the body can manufacture all the fats it needs from other sources such as glucose, this is not actually true. The body uses fats not only as an energy source, but also, crucially, as a component of cell walls and as the insulation that covers all nerve fibers, i.e., the myelin sheath, not just in the brain but everywhere in the body. Two specific kinds of fats, omega-3 fats and omega-6 fats, are called "essential fatty acids" (EFA's) because the body cannot manufacture them. It is essential to obtain them from food sources such as meat, eggs, and fish.
Furthermore, the body cannot produce fat supply in the blood stream "at will." As I have mentioned previously, when insulin levels are high, the subcutaneous fat cells and the abdominal fat cells, as well as the liver, are suppressed from releasing their stored fats. When glucose is available, the fat cells are otherwise engaged in the task of taking up the glucose and converting it into additional fat supplies. The presence of insulin disables the process of lipolysis that is necessary before the stored fats can be released into the blood stream.
2 comments:
Dear Stephanie,
I am interested in the relationship of insulin and ADHD you have discussed.
For someone already with ADHD, do high insulin levels help reduce ADHD symptoms, or do they help cause the symptoms?
Are you aware of any impact insulin levels have on the effectiveness of Ritalin or Dexamphetamine?
I was officially diagnosed with ADHD (Predominantly Inattentive type i.e. ADD) as a 19 year old adult, while at university. This was 12 months ago.
I am also insulin resistant (very high insulin levels when I consume high GI food. Blood sugar remains in normal parameters). I also have moderately elevated triglicerides and very low vitamin D. Otherwise I am in sound health.
I have used both ritalin (6 months) and dexamphetamine (following 6 months) to try and manage my ADHD-PI symptoms, but both are ineffective. My specialist has experimented with low doses, exceptionally high doses, timing of doses, taking with or without food and ensuring foods that impact metabolism and excretion are not consumed, but no benefit in relieving my symptoms have been provided whatsoever. He also remarked I seem to metabolise the drugs considerably faster, and can tolerate significantly higher doses, than his other patients my size and weight (150cm and 44kg).
All I have experienced is side effects such as thirst, heart rate increase, occasional increased sweating. (My current 30mg/day dose of Dexamphetamine tends to make me clean the house a little. Someone mentioned this was a sign of the dose being too high, but any lower nothing occurs. Doses higher than 30mg/day are illegal in Australia, but I don't think I could tolerate any higher anyway).
I have pondered the impact of high insulin on ADHD and the effectiveness of ritalin/dex for a while, and have been researching it. Hence, I stumbled across your blog.
While on Ritalin, I experimented by trialing a three week period where I eat very low GI (allowing insulin levels to be normal), followed by a three week period where I followed a diet comprised almost exclusively of high-GI carbohydrates and sugars and greatly increased food intake. I can't say I observed any difference. When I repeated the experiment after starting Dexamphetamine, I encountered the same negative results. However, I still wonder if there is a link.
I am still taking dexamphetamine, but I am unsure if this is wise due to its ineffectiveness and potential serious effects. My specialist cannot explain why the medication is ineffective and why I seem immune to the thereputic effects. Ritalin, and dexamphetamine in particular (and at the dose I take), are not exactly mild pills.
I am not a scientist (I am a law student), so while I generally understood your post, the specifics are a little lost on me!
If these questions fall outside your field of expertise and cannot answer them I completely understand, and I thank you for taking the time to read this comment. However, any thoughts would be greatly appreciated.
Kind regards,
Anneliese O
Informative post. I would like to say thank you for sharing this article. Get to know about the best clinical diagnostic laboratory services in Kerala.
Post a Comment